
Back in 2014, the NHS produced the Five Year Forward View a wide-ranging project, developed by patients, clinicians and independent experts to create a collective view of how the health service needs to adapt and change over the following five years, in order to cope with the changing needs of our population and continue to improve patient outcomes. As a part of this project the Paperless 2020 initiative was introduced with the aim that the health and care system in England should become paperless at the point of care by 2020
What benefits would a paperless system offer?
Digitising paperwork offers benefits to medical staff, allowing access to clinical information whilst with a patient, so they can easily see a range of useful information including patient notes, care plans, imaging and investigation results – leading to fewer errors, faster results and, ultimately, better care and improved outcomes for patients.
Scanning archives and records from paper, and converting them to a digital format, enables a healthcare organisation to reduce administration, save money and maximise the value of the record data. When information stored in a physical format is digitised, it becomes searchable and easier to cross-reference, offering quicker, cheaper, and safer collection and transfer of data as well as better use of data for research, service improvement and population health management.
In addition to improving the quality of healthcare, scanning also supports the latter part of healthcare’s ‘triple aim’ – better health, better care and lower cost. Document imaging can help organisations achieve significant business efficiencies and cost savings by automating and accelerating processes, controlling and tracking access to data, ensuring the privacy of patient information and producing more accurate audit trails for compliance. Storing data off-site in the cloud also protects it, should there be any type of data storage disaster such as fire flood and theft. Finally, sending a document electronically saves money, time and resources related to costs associated with courier services and photocopying.
Where are we now?
As we move into the new decade, some progress on the Paperless 2020 initiative has been made, but we’re nowhere near achieving that objective. In a huge organisation like the NHS, change can take a long time – due to barriers such as budget cuts, ageing IT equipment, lack of training and lack of expertise in how to make the modifications needed.
Medical records are still largely a mixture of electronic records and paper-based hospital notes. In some cases, there has been additional work in word processing paper notes to be stored on computer – duplicating work and wasting time and resources. Improvement has been lacking in many areas, and progress has been much slower than anticipated.
An example of thiscan be seen at the University Hospital Coventry, a relatively new hospital, completed in 2006. It was built without a physical document storage facility as, at the time, it was expected that medical records would be fully electronic, therefore not requiring a specific place to hold the physical records. However, unfortunately, this is still not the case, and over 850,000 individual patient files, plus 700,000 X-rays and 150,000 archive boxes full of financial and HR paperwork, are being stored at an offsite facility based in Derbyshire, resulting in enormous costs for the hospital to retrieve around 3,500 records every single day. The storage of this paperwork takes up 15,000 square metres and includes thousands of irreplaceable documents, currently at risk of loss, fire and flood.
What can be done?
Although it seems an insurmountable task to move thousands of paper documents, including medical records, x-rays and archives, into digital format, an industry of specialist scanning bureaus, scanners and document management software exist to undertake this task. What’s more, there is also government support for this transition to digital. Health secretary Matt Hancock has recently announced a new digital aspirant programme, to encourage the whole of the NHS to make use of the latest technology. “We’re going to use digital technology to ease the burden on staff, give people the tools and information to manage their own healthcare, and make sure that patient data can be safely accessed wherever and whenever it’s needed across the system,” he said.
“This model of excellence, crucially, will become part of the CQC’s inspection regime so people know they will be assessed against good use of high-quality technology and incentivised to deliver.”
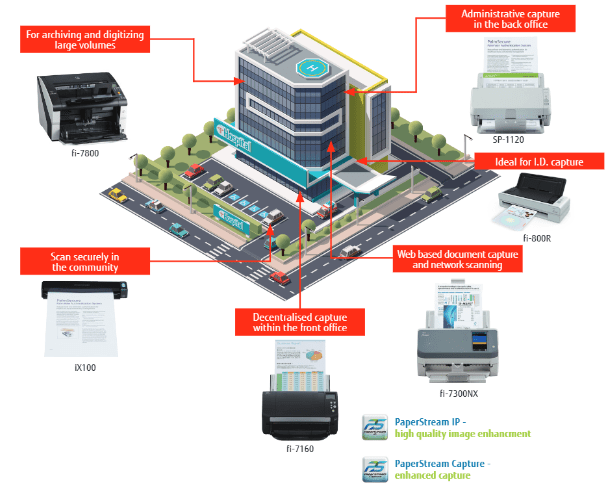
Fujitsu have built a range of scanners, designed with the healthcare industry in mind, to aid the transition to digital. Their range starts with the Fujitsu fi-800R which is a perfect desktop solution for GP and hospital reception desks, with a footprint smaller than the size of an A4 sheet of paper. This tiny powerhouse can scan A4 paper at up to 40 pages per minute, plus ID documents, including passports, up to 5mm in thickness. The next scanner in the range is their ScanSnap iX1500, an easy to use scanner which provides speedy document capture and is useful for everyday document scanning. For high volume scanning, Fujitsu offer the fi-7160. This is the number one, best-in-class deployed scanner in the NHS, designed for high impact batch scanning and reliable performance.
To find out more about Fujitsu scanners, please visit www.fujitsu.com/uk/products/computing/peripheral/scanners/index.html or call 020 8573 4444.

Be the first to comment