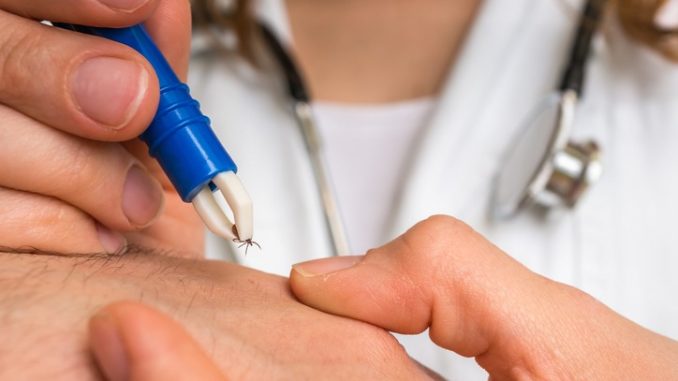
How many patients in your practice have presented with symptoms suggestive of Lyme’s disease recently? Have you noticed an increase in such symptoms? It seems this – potentially nasty – disease is on the march and GPs have a major role to play in alerting their people of how to avoid contact with the little blighters that cause it
Credit: Press Association; The Guardian.
Researchers from the UK and Germany looked at a primary care database holding anonymised records of 8.4 million people registered with GP practices between 2001 and 2012 – about 8% of the general population.
They found that cases of Lyme disease (LD) have ‘increased rapidly’ in the UK and may be three times more common than the current annual estimate, Incidence of Lyme disease in the UK: a population-based cohort study, published on BMA Open, suggests. In this study of GP records Lyme disease was found in every UK region, with Scotland having the highest number of cases, followed by the south-west and south of England. Nice guidelines now state that tics are found in urban parks and gardens across the UK, not just in UK hotspots and abroad. The higher numbers in Scotland could be explained by ‘its wetter climate and popularity as a hiking destination’, the researchers said.
Some 4,083 cases of Lyme disease were detected among 4,025 patients, 56 of whom appeared to have been infected more than once. Of these, 1,702 (41.7%) had ‘clinically diagnosed’ Lyme disease, 1,913 (46.9%) had ‘treated suspected’ Lyme disease, and 468 (11.5%) had ‘treated possible’ Lyme disease.
So these findings show that the annual total number of cases recorded increased almost ten-fold over the period, from 60 to 595, suggesting a UK estimate of 7,738 cases in 2012. However, the current official estimate for the UK is around 2,000–3,000 new cases of Lyme disease annually.
The ‘tip of the iceberg’?
Lyme disease has become the most common tick-borne infection in many parts of Europe and the USA; high rates in nearby countries had prompted fears the current UK estimate was too low.
“From 2009 to 2012, the number of treated suspected cases continued to increase, unlike the number of clinically diagnosed LD cases, suggesting greater caution among the GPs and a willingness to treat the illness early before confirming the diagnosis,” the study states. “Greater caution by GPs is reasonable, as rapid treatment is important to avoid long-term problems.”
“The exact number isn’t so important,” said study author Dr Victoria Cairns, a retired medical statistician from Oxford. “The point is that it’s a lot, and it’s everywhere, and that’s why people should be informed.”
Dr Anne Cruikshank, the Royal College of GPs’ clinical champion for Lyme disease said, “These levels are not a big surprise to those of us who know about Lyme disease. I expect the 8,000 figure may be an underestimate, since the data shows that positive lab results have doubled every five years.”
Professor of medicine at the Mater hospital in Dublin, Dr Jack Lambert, agrees. “I think this is the tip of the iceberg, but this paper is a good step.” Dr Lambert, who treats patients with chronic illness linked to LD, said he was concerned that the Nice guidelines were insufficient for treating people with persistent symptoms. “The Nice guidelines have downplayed Lyme disease. We need to rethink the whole Nice process.” Lyme Disease UK has plenty to say about the Nice guidelines – read this here.
Sally Cutler, Professor of Medical Microbiology at the University of East London, said the methodology and inclusion of patients who were only ‘suspect’ and ‘possible’ Lyme disease cases means the numbers in the study “…are likely to be an overestimation”.
“The authors discuss various factors that could account for the rise in Lyme disease cases, such as increasing public awareness of the disease and, therefore, more people visiting a health professional and being diagnosed. Alternatively, climate change might enable ticks to remain active for longer, lengthening the time available for a tick to infect a human.
“For such reasons, continued observation is a priority… This study was reassuring in that suspect cases were receiving benefit of doubt from their GPs, and were being treated.”
Signs and symptoms
The bacterial infection that does the damage is spread to humans via bites from infected ticks. Symptoms can include a circular red rash, often described as a ‘bullseye on a dartboard’; this rash usually appears around three-to-30 days after being bitten. The affected area of skin will be red, the edges may feel slightly raised and some people may develop several rashes on different parts of their body.
Unfortunately, not everyone has such an obvious and easy-to-spot giveaway symptom; around one-in-three people with Lyme disease won’t develop this rash. Some people get ‘flu-like symptoms instead of the rash in the early stages – things such as, such as tiredness, muscle pain, joint pain, headaches, a high temperature (fever), chills and neck stiffness.
Dr Cairns says the disease has often been called ‘the great imitator’ because it mimics other symptoms. “…that’s really the big problem with Lyme disease – some people don’t get diagnosed quickly enough and then they go on to get long-term problems.”
If not treated promptly with antibiotics Lyme’s disease can develop, potentially causing pain and swelling in joints and nerves, as well as heart problems and trouble concentrating for years after.
One celebrity victim, former England rugby captain Matt Dawson, was bitten by a tick in 2016. He developed feverish symptoms after visiting Chiswick Park in London and was later diagnosed with Lyme disease; he says was struggling to exercise as much he would like even two years after.
The more serious symptoms may develop several weeks, months or even years later if Lyme disease is left untreated or is not treated early on. These can include:
- pain and swelling in the joints – inflammatory arthritis;
- problems affecting the nervous system such as numbness and pain in limbs, paralysis of facial muscles, memory problems and difficulty concentrating;
- heart problems such as myocarditis, pericarditis, heart block and heart failure
- meningitis – which can cause a severe headache, a stiff neck and increased sensitivity to light
Some of these problems will slowly get better with treatment, although they can persist if treatment is started late. A few people with LD go on to develop long-term symptoms similar to those of fibromyalgia or chronic fatigue syndrome.
Prevention is better than cure
Experts say prevention is the best way to ward off the disease as there is currently no vaccine available to prevent LD. The best way to prevent the condition is to be aware of the risks when you visit areas where ticks are found and to take sensible precautions.
You can reduce the risk of infection by avoiding being bitten by:
- keeping to footpaths and avoiding dense vegetation and long grass when out walking;
- wearing appropriate clothing in tick-infested areas – ie. a long-sleeved shirt and trousers tucked into your socks;
- wearing light-coloured fabrics that may help you spot a tick on your clothes;
- using insect repellent on exposed skin – and on clothes;
- showering and inspecting your skin for ticks, particularly at the end of the day, including your head, neck and skin folds (armpits, groin and waistband) – remove any ticks you find promptly;
- checking your children’s head and neck areas, including their scalp;
- making sure ticks are not brought home on your clothes;
- checking that pets do not bring ticks into your home in their fur.
If you find a tick you should:
- use tweezers to pull the tick off as soon as possible – trying not to squeeze its body;
- clean the area with antiseptic;
- put the tick in a zip-lock bag so it can be tested;
- wash all clothes at a high temperature;
- check the rest of your body for further ticks;
- draw around any rash with a pen and take photos of any changes.
If you notice a rash or become unwell, see your GP immediately and raise your concerns about Lyme disease; be aware of ‘flu-like symptoms
Primary care, changing the landscape on Lyme
GPs are doing a great job in identifying potential cases of Lyme disease, as this research shows. The data showed that the number of diagnoses increased almost tenfold over the period studied. This, the researchers said, was partly down to increased caution by GPs and greater public awareness.
“This is really just showing there are many more cases than previously, officially estimated,” says Dr Cairns. “I think GPs certainly know about it; the issue is really for the public to know so that they go to the GP to get diagnosed.”
GP practices can continue to help reduce the harms which Lyme disease can bring by making their patients alert to the dangers and aware of the steps they can take to keep themselves safe; it is especially important to run a Lyme-awareness blitz in your surgeries at this time of year when your patients will be taking their holidays both at home and abroad. With ticks widespread across the UK and Europe your community needs to get the message regardless of where they intend to travel to.
Dr Cairns says she hopes the new data will encourage the public to take more preventive measures, and bring about faster diagnoses. “The main thing that should come out of [this work] is to be on the alert. There’s no need to panic, the treatment works – but if you don’t get it in time you might have some long-term problems.”
LDUK can help practices with awareness-raising videos and packs and the RGCP has developed a Lyme Disease toolkit and course.
There’s no need to panic, the treatment works – but if you don’t get it in time you might have some long-term problems.
Don’t forget to follow us on Twitter, or connect with us on LinkedIn!

Be the first to comment